Ending HIV transmission by 2030 in doubt due to ‘stark’ Tory government failures: ‘It’s really dire’

SInce Rishi Sunak appointed Steve Barclay as the new health secretary sexual health services have been calling on him to ramp up funding. (Getty)
In 2019, then-health secretary Matt Hancock committed to ending new HIV transmissions by 2030.
It was a seismic moment, but three years on, doubts are starting to creep in. HIV charities and activists are concerned that the goal is getting further out of reach with each passing year.
That’s due to a range of obstacles, from the effects of the COVID-19 pandemic to the monkeypox outbreak – but it’s also down to a lack of resources and a general reluctance on the part of the government to take the radical action that’s needed.
Richard Angell, campaigns director at the Terrence Higgins Trust, tells PinkNews that it’s now “possible but not probable” that the UK will end new HIV transmission by 2030.
Things are moving in the right direction – the introduction of opt-out HIV testing in some emergency departments has been a game changer – but more needs to be done.
“The opt-out testing that is so clearly working in London, Brighton, Blackpool and Manchester is not being run in other areas,” Angell says.
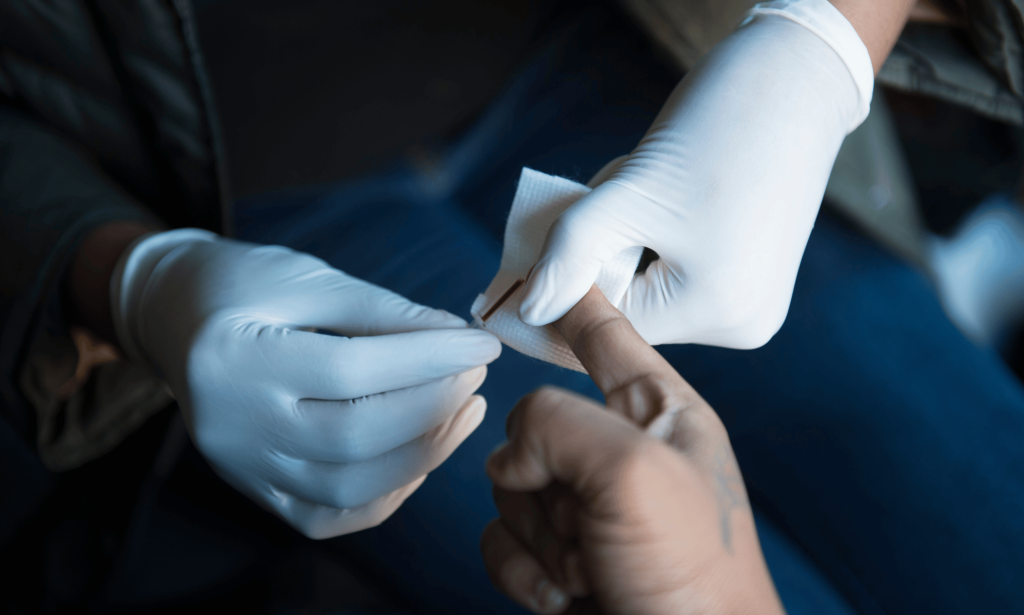
“Government guidance is that everybody who goes to A&E in a high prevalence area should be tested automatically for HIV. They’re already taking your blood, there should be an automatic HIV test.
“The funding is only there to do that in the very highest prevalence areas, but there are places – whether it’s Luton, Leicester or Leeds, whether it’s Bournemouth or Birmingham, Sandwell or Southampton – where this testing is not yet happening.”
The fact that it’s working so well makes it so stark that it’s not working so well in those next tranche of cities.
Expanding opt-out testing is vital because it ensures people with HIV get effective treatment sooner, which means they can’t pass the virus on.
“There’s some really good things happening and that investment last year in opt-out testing was a hugely welcome step forward. The fact that it’s working so well makes it so stark that it’s not working so well in those next tranche of cities.
In some ways, the HIV sector has been “a victim of its own success”, Angell says – the government likely never expected opt-out testing to be as successful as it has been.
“We know in just 100 days, having just spent £2.2 million, we found 128 people living with HIV, 65 people who were previously lost to care. That’s 200 people not having HIV attack their system and 200 people who now can’t pass on the virus, and it’s probably saved the NHS between six and eight million pounds.
“It’s a huge success and I think, to be honest, the system wasn’t expecting it to be that categoric that quickly.”
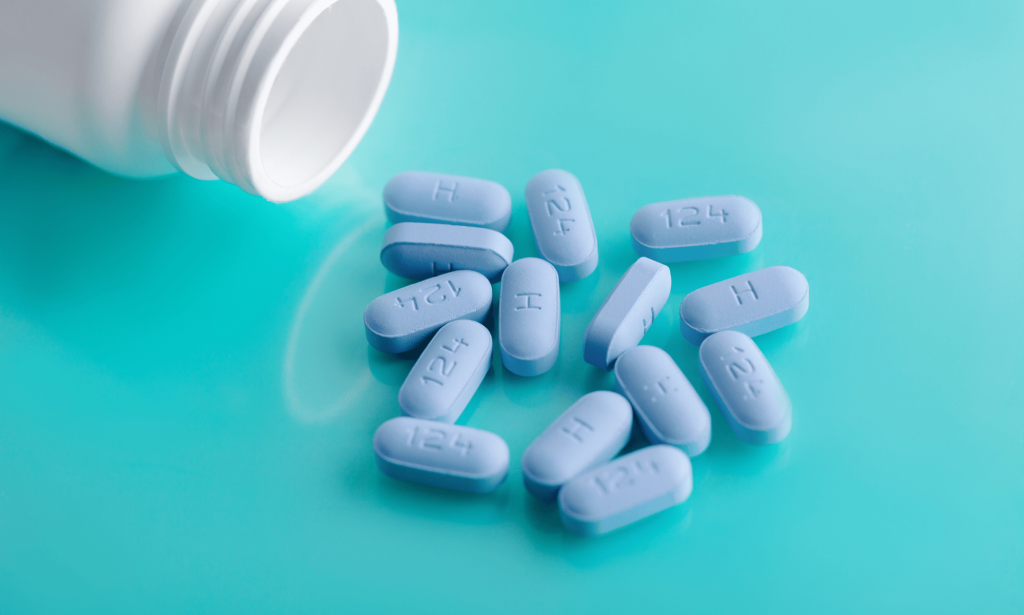
PrEP is key to ending HIV transmission
Claire Dewsnap, president of the British Association for Sexual Health and HIV (BASHH), says the 2030 goal is still “possible”, but it will only happen if testing is expanded and PrEP – a drug that prevents a person from contracting HIV – is better utilised.
“We need to make sure that everyone understands PrEP. I think there should be a national campaign about it – a bit like the tombstone. Everyone recognises that. We need a similar thing around the 2030 goal so that it’s in everybody’s mind.”
She would also like to see better training across the NHS to make sure those who are genuinely at risk of contracting HIV are getting access to PrEP as quickly as possible.
“The experience in Australia was that it’s the people on the edges of eligibility that end up with HIV. It’s not the people who are like, ‘yes I go to chemsex parties’ – those people get PrEP.
“It’s the people who are just on the edge of being in or out of the criteria, people who might not have been having sex for six months but are planning to have it now. Those are the people who are not getting PrEP, and we need to make sure those are the people we focus on in the next couple of years.”
Dewsnap’s message to the government is clear: the 2030 goal will only be achieved if there’s a well-thought-out strategy.
“If you want this to happen you’re going to have to think of a national strategy with appropriate funding for localised improved testing and in particular reducing late diagnosis rates,” she says.
“The second thing that’s got to happen is you have to increase access to sexual services and make PrEP available outside of sexual health services. For that to happen there really is going to have to be some kind of strategy. It’s not going to happen on its own.”
Inequality and stigma are standing in the way
It’s not all about the UK either – the world should be moving towards eliminating HIV transmission, but global barriers remain in the way of progress, according to Anne Aslett, CEO of the Elton John AIDS Foundation.
“COVID, global energy costs and conflict such as the war in Ukraine have all had an impact on our ability to realise an end to the AIDS pandemic,” Aslett says.
“But much more than this, the vulnerability of certain people in society, driven by inequality, stigma, discrimination and even criminalisation is what is really hampering our progress.
“The global community has the science to stop new HIV infections and AIDS deaths right now. If we can’t embrace the idea that that access to that science, compassionately and without judgement, should be available to all, we will struggle to meet the 2030 goal.”
If the 2030 goal is to be reached, there must be a “clear-eyed acknowledgment of the scale of the problem and for whom”, Aslett says.
“Globally, people from vulnerable communities – including LGBTQ+, people who use drugs, sell sex or are incarcerated – make up 70 per cent of new infections,” Aslett says.
“Yet in many parts of the world these populations are not counted: they are invisible and marginalised. This means the resources needed simply are not allocated.”
The global community must tackle “punitive laws and policies” that prevent people from getting tested for HIV.
“Florida’s so-called ‘Don’t Say Gay’ bill and new legislation in the Russian Duma make it more and more dangerous for LGBTQ+ individuals to be open about their status and needs,” Aslett says.
“We also need to find affordable, scaleable ways to reach people with the services they need. COVID has taught us how valuable online, digital services can be in supporting people effectively and confidentially and linking them to PrEP, HIV testing and treatment.”
While most are optimistic that the 2030 goal could yet be reached with some hard work, Greg Owen, co-founder of iwantPrEPnow.co.uk, has less hope for the future.
“That 2030 goal that the government made, it’s just not going to happen. Come on, it’s absolutely not going to happen,” he says.
The problem’s roots lie in the fragmentation of the health system, he argues, which means people can “kick responsibility” for ending HIV transmission to different departments.
I would like to put a positive spin on it but I can’t.
“What really needs to happen is we need to wake up and wise up. The system was creaking anyway, COVID didn’t make things any better, and then we got over COVID and we were faced with a second epidemic outbreak of monkeypox.”
The situation, Owen says, is “really dire”.
“I would like to put a positive spin on it but I can’t.
“Something needs to happen and I think the only thing that can happen at this point is to vote out the Tory government and have new leadership, because that’s the only way to secure change.”

