Experimental twice-a-year HIV treatment shows early promise in new study
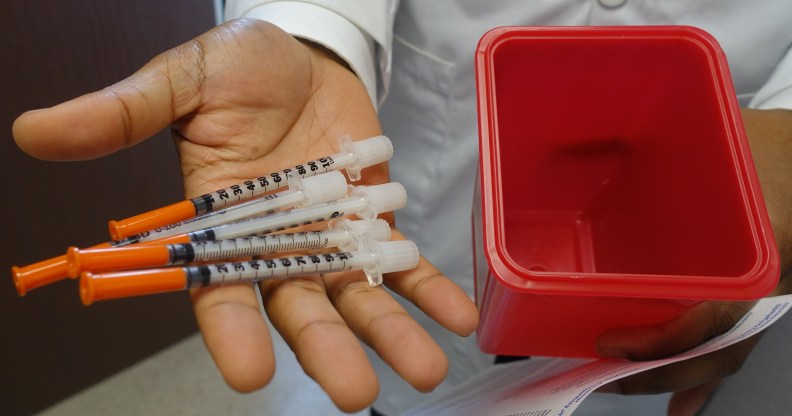
HIV
Early results from a small study suggest a biannual injection could become a safe and simple antiretroviral treatment for HIV.
At the moment, those living with HIV can take antiretroviral treatments to reduce the amount of HIV in their blood to a very low, or undetectable, level.
Such treatments are typically daily pills and, while sorely needed, have their fair share of problems, including the cost of treatment (for those without publicly-funded healthcare or insurance).
Missed pills give the virus the chance to become resistant to treatment, while research suggests people overwhelmingly prefer monthly injections to daily tablets.
But lenacapavir, an injection being developed by Gilead Sciences, has shown early promise in what scientists have dubbed a “breakthrough innovation in HIV research”.
In two new studies presented at the International AIDS Society Conference on HIV Science, researchers found the drug dramatically decreased people’s viral loads, or the amount of virus a person has inside them.
Getting this number to undetectable levels is key. And a pair of findings from two studies have found when lenacapavir is injected every six months and taken with other tablets, it achieves just that.
Injectable drug is a ‘breakthrough innovation in HIV research’
Lenacapavir works by preventing the virus from shedding the hard shell casing, known as a capsid, around its genes.
The CAPELLA study, Gilead Science said in a press release Saturday (17 July), tracked 72 people who had been living with HIV for more than 24 years.
In a particularly exciting finding, around 80 per cent of those living with HIV whose therapy was not working and who had resistance to drugs saw their viral loads decrease to undetectable levels after the first shot.
This is a huge leap in terms of the options those living with HIV have to choose from, researchers said, noting that the twice-yearly injection paves the way for a more manageable regime.
A separate study, known as CALIBRATE, found in its second phase data that when lenacapavir is injected and taken with emtricitabine/tenofovir alafenamide (TAF) tablets, 94 per cent of participants achieved an undetectable load.
Unlike CAPELLA, the second study involved 182 people new to HIV treatment.
Experts stressed that while the preliminary results are encouraging and the drug was shown to be effective on a wide range of people living with HIV, more work has to be done. CALIBRATE, for example, was not designed as a licensing trial so further studies are vital.
“Despite the advances in treating HIV infection, there remains an unmet need for treatment options for people who struggle with multi-drug resistance,” said Jean-Michel Molina, professor of infectious diseases and head of the Infectious Diseases Department at the Saint-Louis and Lariboisière Hospitals.
“As a physician, it’s frustrating to have limited options for these patients who are at greater risk of progressing to AIDS.
“The CAPELLA results are exciting as they demonstrate that an undetectable viral load is achievable in a patient population that has typically had challenges with viral suppression over the course of their journey living with HIV.”
“Lenacapavir is a breakthrough innovation in HIV research,” Frank Duff, senior vice president of Gilead Sciences, said in a statement.
“If approved, it has the potential to become a cornerstone of future long-acting HIV regimens.”

