Ireland to overhaul its ‘dehumanising and humiliating’ care for trans people

Ireland has revealed plans to improve its treatment of gender dysphoria. (Credit: Getty/Envato)
Ireland is planning to refine its care for gender dysphoria, a Health Service Executive (HSE) official has announced.
Chief clinical officer, Dr Colm Henry, presented a report to the HSE executive management committee, outlining how the new model will be created.
He explained that, because of reported developments in the understanding of gender dysphoria, the HSE intends to create a multi-disciplinary team to help update its treatment model.
“The team will be led by a clinician from a relevant speciality, whose role will be to load this process,” he told The Irish Times.
“The epidemiology of gender dysphoria is changing, and will continue to do so. We are aware of 15 other countries who are looking at their models of care and we are doing so too.”
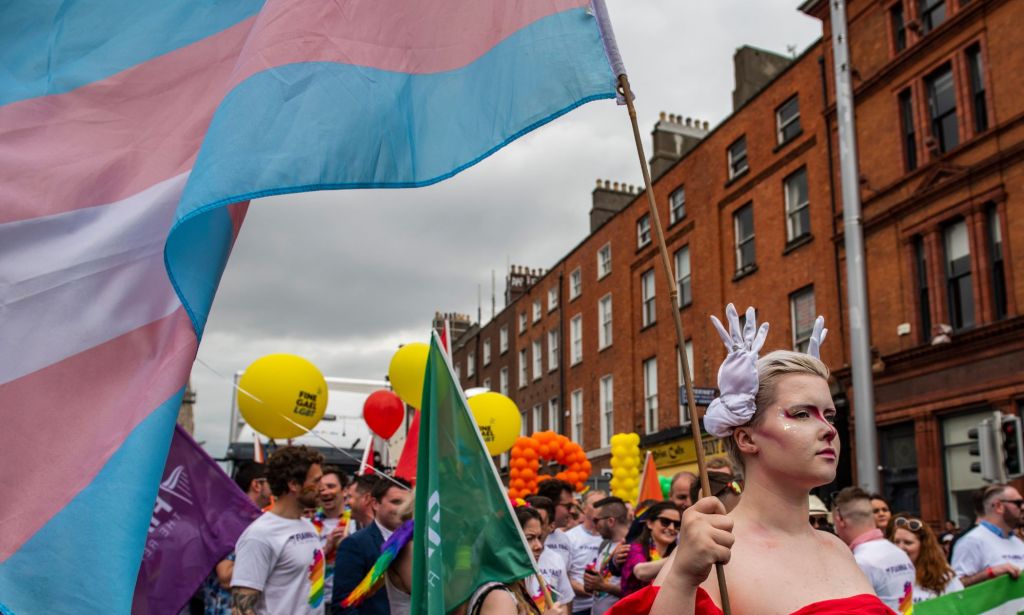
Gender dysphoria is defined by the NHS as a “sense of unease” about a person’s assigned gender identity, which can cause depression and anxiety.
It is usually treated by beginning hormone-replacement therapy (HRT) or with gender-affirming surgeries.
Younger patients who experience gender dysphoria are given physically reversible puberty blockers but are unable to undergo gender-affirming surgeries until they turn 18.
Currently, Ireland predominantly refers gender-dysphoria cases to the National Gender Service (NGS) where hormones can be administered.
Henry’s guidance to establish an improved model of care comes amid rising waiting times, with some people having to wait years before their first NGS appointment.
Ireland rated worst provide of trans healthcare in Europe
A report in November 2022 revealed that more than 1,200 people were on the waiting list to access gender-affirming care in Ireland, and, in 2022, the country was the lowest-ranked nation in the European Union when it came to trans healthcare.
“We will be establishing a new model of care: [a] multi-disciplinary model of care, covering primary, secondary and tertiary services, to update and replace [the current system],” the medic said.
“The objective is to have an entirely domestic service.”
After surveying experts across 27 countries, Transgender Europe, a group of organisations that combat discrimination against trans people, found that Ireland’s healthcare provisions for trans people warranted just one point out of a potential 12.
The survey revealed that the waiting time for accessing healthcare could range “between 2½ and 10 years.”
A statement from Trans and Intersex Pride Dublin (TIPD) read: “With only one clinic in Ireland for trans adults, the current waiting [time] to be seen is estimated to be six years or more.
“When you’re finally seen, you’re put through a dehumanising and humiliating assessment and asked invasive questions.”
To make matters worse, trans people are constantly denied HRT, TIPD added.
Reasons given for the refusal of HRT included the trans person “having a diagnosis of autism, attention deficit hyperactivity disorder, or a personality disorder,” or because they are “on social welfare”.
TIPD went on: “Trans people should be empowered to make decisions about their transition themselves.”
The Cass Review prompts Tavistock and Portman closure in UK
An interim review by Dr Hilary Cass in 2022 prompted similar calls to revamp trans youth healthcare in the UK.
As a result, the Tavistock and Portman NHS Foundation Trust, in north west London, which deals predominantly with trans youth care, is to shut down in favour of a “holistic and localised approach”.
But the clinic’s eventual demise has left activists worried about whether regional replacements will be as effective.
In her report, Cass wrote that a “comprehensive patient and family-centred service” could ensure trans youth are able to get the healthcare they need “as an individual”.
The report said the “great amount of change” in the awareness and understanding of gender dysphoria prompted the recommended reform.
Cass added that the increasingly divisive fight for trans rights means that, because there is “more knowledge” in the public eye, more people are seeing it as an option.
“The review is not able to provide definitive advice on the use of puberty blockers and feminising/masculinising hormones at this stage,” she said.
“[This is] due to gaps in the evidence base. However, recommendations will be developed as our research programme progresses.”

